Medical Emergency Team Action Plan
The survival rate for individuals who experience cardiac arrest inside a hospital is not great—only about 20%. The development of a Cardiac Arrest System of Care was a reaction to this low rate of survival. They found that before the cardiac arrest, four out of five individuals experience noticeable differences in their vital signs. By identifying those patients who show signs of cardiac arrest, such individuals can be treated with proper ACLS protocols before it is too late.
Cardiac Arrest Teams have traditionally been assigned to cardiac arrest patients. The Code Blue immediately calls these teams after an active cardiac arrest has been detected. However, it was discovered that Cardiac Arrest Teams didn’t improve survival rates—in fact, hospitals without Cardiac Arrest Teams had survival rates similar to those that were staffed with these teams. Because of this, Cardiac Arrest Teams have been replaced with Medical Emergency Teams (METs) or Rapid Response Teams (RRTs). Anyone can call for the RRT/ MET if there is any concern by the patient, a health care provider, or a family member.
RRTs/METs keep a close eye on patients to treat their cardiac arrest before it occurs, instead of waiting for the cardiac arrest to take place. Composed of nurses, physicians, and family members, these teams work tirelessly to find signs of an impending cardiac arrest.
RRT/MET Alert Criteria
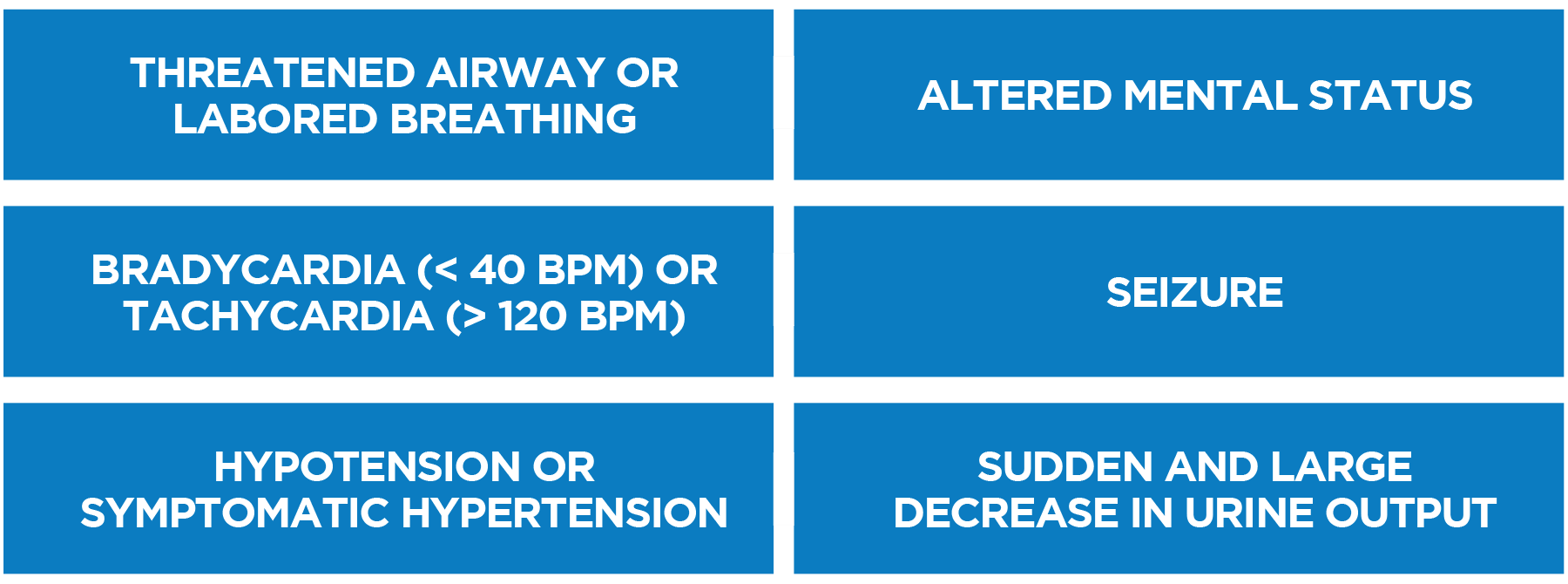
Figure 19
Hospitals that staff RRTs/METs experience fewer ICU transfers, fewer cardiac arrests, improved survival rates, and quicker patient recoveries.
