Why You Should Take the PALS Pretest Right Now
Why You Should Take a PALS Pretest

by Greta Kviklyte
Life Saver, AMC
Co-authored by Kim Murray, RN, M.S.
posted on Jul 23, 2018, at 5:14 pm
Children are susceptible to unintentional injuries at a higher rate than adults. According to the Centers for Disease Control and Prevention (CDC) more than 12,000 children up to age 19 lost their lives from unintentional injuries and ailments. Sudden cardiac arrest (SCA) is included in these statistics. This is due to the presumed prevalence of SCA among children and teens with an active lifestyle, such as being involved in athletics. Due to the risk of unintentional injury and trauma to children, it is imperative health care providers and professionals understand how to perform Pediatric Advanced Life Support (PALS).
We offer Online PALS Certification and Renewal
Thus, completing a PALS pretest to check your life-saving skills can serve as a refresher course and means of study for recertification or initial certification of pediatric care skills.
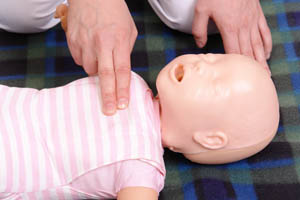
Why a PALS Pretest Is Valuable
Among children, the cause of cardiac arrest can vary from injuries to ingestion of toxins and poisons. Drowning, burns, and falls may contribute to cardiovascular issues, and the threat of electrocution, even in homes with child-proof electronics and electrical devices, such as electrical outlets, remains.
Although the CDC calculates mortality rates for SCA in terms of the whole public, including children, a bit can be ascertained by looking at the statistics. According to UptoDate.com, approximately 1,500 children under age 26 die from SCA annually. Paired with the CDC’s statistic of 12,000 childhood deaths following fatal injuries, approximately 12.5 percent of all childhood mortality cases are linked to SCA.
The problem does not end there. According to AHAJournals.org, as few as one-third of children that suffer an out-of-hospital arrest are provided with CPR until trained health care professionals arrive. This is associated with a higher risk of mortality due to the six- to 15-minute window between contacting emergency medical services and their arrival.
Even bystander hands-only CPR can increase chances of survival. However, the shocking statistic regarding the lack of care between recognizing a problem and getting help for the 33 percent that never receives bystander assistance emphasizes why quality skills in PALS are key to survival for infants, children, and teens.
The Importance of Frequent PALS Reviews
Completing the PALS pretest is of the utmost importance. Having the right skills and understanding the intricacies of PALS will mean the difference between life and death for children suffering from cardiac arrest or other trauma. Also, mistakes made in the course of providing PALS could result in additional consequences, including brain damage, limited mobility, and poor quality of life among survivors. PALS training counts toward continuing education units (CEUs) for health care providers, including nurses. CEU minimums are necessary for the renewal of licensure and employment. Depending on the employer, state standards for PALS certification, which are typically two years, may vary. For example, nurses working in pediatric acute care may be required to renew PALS certification every year, if not more frequently.
The demand for high-quality skills in PALS is not exclusive to acute care settings. Health care providers in medical-surgical care and even physician offices need to know how to perform PALS. Although trauma and unintentional injury make up a large portion of cardiac arrest cases, an incident can occur in any setting. This could be the exposure to an allergen or a reaction to medications. Remember children may not exhibit allergies to certain medications or materials until they come into contact with the allergen.
For example, a child could presumably enter anaphylactic shock upon receiving a standard childhood vaccine.
Among care professionals in critical care, the frequency of PALS administration varies as well. Consider this; the first step of treatment for cardiac arrest, diminished neurological capacity, drowning, or other issues occurs in the pediatric emergency department. In critical care, children are more likely to be medically stable. However, the simplest of days can turn chaotic when a child experiences one of the events contributing to cardiac arrest or need for PALS administration. For care professionals that have not recently renewed their PALS certification, ability to provide high-quality care decreases. The rectification of these problems is simple; health care professionals need to test their skills often and complete recertification courses frequently.
Common PALS Mistakes and Frequently Missed Questions on the PALS Pretest
Common PALS mistakes are similar to the mistakes made by health care professionals in performing ACLS. However, the nature of providing care on varying age groups, ranging from neonatal care settings to adolescents, requires in-depth knowledge of the typical growth and anatomy of a child for the given age, as well as an understanding of the variances in PALS standards for the age group. These mistakes can be broken into three primary categories:
Failure to Get Proper Help
- Failure to recognize when to activate the emergency response system. Knowing when to activate the emergency response system is key to increasing chances of survival among children. As a child, the body is less able to compensate for sudden changes in cardiovascular output. Thus, activating the response system immediately, including calling for help at once, is essential to reducing mortality.
- Lack of understanding regarding traumas and their associated CV effects. Due to the increased risk of trauma and unintentional injury of children, health care professionals must also understand the types of traumas children are likely to suffer. As noted by the CDC, drowning is the most common cause of death for young children ages one to 14. The care measures for drowning differ from those for other traumas, such as being hit by a moving vehicle. Think of the differences in approaching a child that has run into the street chasing a ball versus a drowning victim. The ball case may include loss of blood resulting in hypovolemic shock, and the drowning case is hypoxia.
- Not considering the presence of family members, parents or others with the affected child. A key consideration in providing PALS for children focuses on addressing panicked parents and family members. A childhood trauma or cardiac arrest is an intense situation, and health care professionals must be capable of explaining what is happening while administering care. In other words, communication skills become a priority for both the patient and those that care for him or her.
Mistaking ACLS Guidelines for PALS Guidelines
- Administering incorrect medication dosages for the child’s weight and age. Not understanding minimum and maximum mediation dosage reasoning is a common mistake among 45 percent of those who take the pretest. For instance, the 2015 updates to the PALS algorithm, reports the American Heart Association, dictate a 0.02 mg/kg dose of atropine is appropriate for premedication for emergency intubation when there is a higher risk of bradycardia among infants and young children. Administering the incorrect dosage could lead to an increased risk of bradycardia. Similarly, administering this dosage of a different medication, mistaking medications, could result in additional complications and trouble stabilizing the child.
- Common mistakes in identifying areas to take a pulse on an infant or child. Children and infant pulses can be difficult to detect in the standard wrist position or neck. Furthermore, trauma contributing to the cardiac arrest can make ascertaining a pulse on a smaller child more difficult. As a result, the brachial pulse is the most reliable area to take a pulse on infants and young children. Yet, up to 28 percent of pretest takers miss the question regarding where the brachial pulse is located. For reference, it is the located on the inside of the upper arm, directly between the biceps and triceps muscles.
- Poorly assessing mental state or being unable to communicate in terms a child understands. There are two general standards for assessing the mental state and overall health of the child when providing treatment. These include the (Alert, Voice, Pain or Unresponsive) AVPU scale and Glasgow coma scale (GCS). Although the GSC is a more intense scale, capable of identifying the exact treatment needs and likely causes, its intensity makes it a lesser choice in providing care. The AVPU is the easiest scale to use for children that are unresponsive and family members that are incapable of providing information regarding the incident. Furthermore, delays in providing care while trying to use the GSC may result in additional risk.
Lack of Medical Knowledge Mistakes
- Failure to treat the reversible causes of arrest. As with ACLS, knowing the reversible causes of arrest is an integral step in providing the right treatment. To recap, the list is made of up terms that start with the letters, “H and T.” The list includes hypovolemia, hydrogen ion buildup (acidosis), hypothermia, hypoglycemia, hypoxia, and hypo- or hyperkalemia. The “T” causes includes a cardiac tamponade, tension pneumothorax, toxin buildup (poisoning), and pulmonary or coronary thromboses. The cause determines the course of action in the PALS algorithm. In fact, 29 percent of those taking the pretest chose an incorrect answer when presented with reversible and nonreversible causes of cardiac arrest.
- Being unable to recognize arrhythmias and identify the best course of action to the treat such issues. The ability to recognize arrhythmias is also important. Certain rhythms may mask causes of cardiac arrest, and others can appear as mirror images. Ventricular fibrillation and atrial fibrillation look similar, but the treatment varies. As a result, refining skills in recognizing the rhythms on an electrocardiograph (EKG) is essential to providing the proper care.
- Spending too much time trying to establish a venous access. This problem is identical to the problem noted with understanding the components of ACLS. In infants and young children, veins may be more likely to “roll,” and finding a vein capable of sustaining a catheter is difficult, especially among children in pain and moving frantically. As a result, establishing a venous should be a fast process, including the use of an intraosseous access if venous access cannot be immediately established. Although this may cause additional pain to the child, the goal of survival takes priority.
- Damaged equipment or lacking access to necessary equipment. Although not specific to a health care professional’s medical knowledge, damaged or insufficient equipment goes back to the basic duties of checking for stocked supplies and verifying the contents of the Crash Cart for use in emergencies requiring administration of PALS. As a result of damaged or missing supplies, mortality risk increases. Essentially, the child in need of care is delayed in receiving the best care possible, so chances of survival decrease, similar to the decreased chance of survival in outside environments.
Put Your PALS Skills to the Test Now
An emergency is not the time to reconsider your understanding of the PALS algorithm and its standards. While no one wants to think about the possible risk of mortality among children, it is an occurrence that requires preparation, not unlike the very nature of nursing school. Rather than hoping your skills can rise to the occasion, put them to the test with our life-saving PALS skills pretest today.
Have you been part of the team responding to a child in distress, or have you made mistakes in administering PALS? Don’t keep it a secret. Share your experiences, keeping HIPAA requirements in mind, and help us become a more effective team and group of caregivers. Also, share this post on social media, and don’t forget to consider renewing your other life-saving credentials today.




