Medical Problems
Medical problems can range from very minor to life-threatening emergencies. Rescuers trained in first aid must be prepared to respond appropriately.
BREATHING PROBLEMS
Breathing problems can arise from underlying lung diseases such as asthma or emphysema, as well as from illnesses such as pneumonia. Be aware that the other body system problems such as heart attack, stroke, seizure, or anxiety can all result in breathing issues as well.
Signs of a breathing problem include fast or shallow breathing, noisy breathing, producing unusual sounds, or the inability to talk due to breathlessness. Persons with asthma often make a musical sound when breathing, which can be heard as wheezing. Severe allergic reactions can also cause wheezing. High-pitched sounds during inhalation may suggest a partial blockage of the upper airway.
Persons who have asthma or chronic lung disease are generally familiar on how to use their breathing medications. Common medications include albuterol and atrovent inhalers. The use of a spacer (a tube attached to the inhaler that holds the medication until the person breathes it in) can improve the effect of these medications. A person in severe distress may be unable to properly use their inhaler. Call 911 if the person appears in significant distress.
Technique for using an inhaler:
- Shake the inhaler canister.
- Place the opening of the inhaler into the spacer if available.
- Instruct the person to fully exhale.
- Place the spacer or inhaler into their mouth.
- Simultaneously have the person inhale slowly and deeply while pressing down on the top of the inhaler canister.
- Instruct the person to hold their breath for up to 10 seconds if possible.
- Be prepared to repeat if respiratory problems persist.
- Stay with the person until the symptoms improve or until emergency response arrives.
 Figure 5
Figure 5



ALLERGIC REACTIONS
Allergic reactions can arise from insect stings, from adverse reaction to foods and medications, or from environmental triggers such as pollens, dust, or chemical fumes. Bee, wasp, or hornet stings can produce rapid and potentially fatal reactions while common food triggers include nuts, eggs, and fruits. Symptoms may be mild, such as itching and hives, or severe causing life-threatening swelling of the airway, lips, and tongue.
Epinephrine can be a life-saving medication and should be given at the first sign of a severe allergic reaction. Commercially available epinephrine pens, such as EpiPen®, are simple to use.
The basic instructions for using epinephrine pens are as follows:
- Form a fist around the pen and remove the safety release cap (Figure 5a & 5b).
- Place the orange end of the pen against the outer mid-thigh (with or without clothing) (Figure 5c).
- Push down hard until a click is heard or felt, and hold the pen in place for 10 seconds (Figure 5d).
- Remove the pen and massage the injection site for 10 seconds.
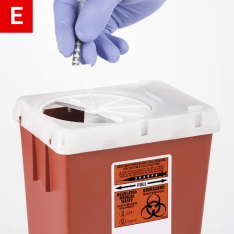
- Properly dispose of the used device in a sharps container (Figure 5e).
- Note the time of the injection.
- Seek medical care.
Antihistamines, such as diphenhydramine (Benadryl®), are also important in the treatment of severe allergic reactions. Be aware that epinephrine will wear off, and the persons receiving an injection should be evaluated at an appropriate medical facility.
HEART DISEASES
Heart disease remains the leading cause of death in the United States. Your prompt actions can mean the difference between life and death during a heart attack. If the person is experiencing a heart attack, blocked blood flow to the heart tissue results in muscle death. (Keep in mind the mantra: Time Is Muscle.) Prompt response and medical attention is critical in limiting damage to the heart muscle.
Chest discomfort can be described as ache, pressure, squeezing, or crushing. Certain persons such as women and diabetics are less likely to have classic signs of a heart attack. These individuals may simply experience nausea or unexplained fatigue. Shortness of breath could be the only sign of an impending heart attack for some individuals.
Denial often adds a significant delay in seeking care. Many persons argue that they are too young or too healthy to have a heart attack. Even those with minimal risk factors can suffer a heart attack.
Aspirin keeps blood clots from growing larger and may reduce the severity of a heart attack. If there is no true allergy to aspirin, no serious bleeding, and no signs that suggest a stroke, give aspirin to the person.
When caring for a person who may be having a heart attack, do the following:
- Keep the person and yourself calm.
- Have the person sit or lie down.
- Activate the emergency medical system by calling 911.
- Give 2 to 4 baby aspirins or half to a full adult aspirin tablet. Make sure the aspirin is not enteric coated.
- Be prepared to administer CPR. Heart attacks can become fatal quickly.
A heart attack is a life-threatening medical emergency. Persons with symptoms of a heart attack should be transported to the hospital via emergency medical services (EMS). Do not allow a person suspected of having a heart attack to drive themselves to the hospital. Encourage the person to wait until EMS arrives. If they refuse, find someone to go with them.
FAINTING
Fainting is a common reaction to a variety of conditions. Individuals may faint at the sight of blood or during periods of intense emotional stress. More serious conditions, such as an abnormal or erratic heart rhythm, can also cause fainting. Also, severely dehydrated persons may faint when standing up suddenly. The body’s reaction to the decreased blood flow to the brain causes the person to pass out. By lying down, blood flow to the brain is improved.
When caring for a fainting person, do the following:
- Ensure safety of the scene.
- Help the person lie down.
- Elevate their legs if possible.
- If there is no rapid improvement or the person becomes unresponsive, call 911.
A person can also faint while seated in a chair. In this case, help them to the floor. Be aware of the potential for injury if the person has fallen. If the person does not quickly regain consciousness, immediately call 911. Keep in mind that fainting can be caused from a wide range of problems, some of which can be life-threatening. If you are unsure of the cause of fainting, call 911.
LOW BLOOD SUGAR IN PERSONS WITH DIABETES
Diabetes affects a person’s ability to regulate blood sugar. Fluctuations in blood sugar in either direction can produce symptoms. Persons with diabetes can experience low blood sugar due to illness, stress, skipping meals, or taking too much insulin.
Low blood sugar can cause altered states of consciousness such as agitation, confusion, and loss of consciousness. Very low blood sugar can result in excessive tiredness, weakness, and even seizure-like activity.
When dealing with a person suspected of having low blood sugar, do the following:
- Give them a sugar-containing beverage, such as fruit juice, milk, or a soft drink.
- Encourage them to sit or lie down.
- Call 911.
- If their symptoms improve, encourage them to eat.
Glucose gel and tablets are available and are a good way to quickly increase blood sugar. Alternatives to gels and tablets include packets of sugar, honey, or jelly from restaurants which may be readily available. Consider keeping any of these in the first aid kit.
If a person with diabetes is unable to sit up or swallow safely, do not give them anything to eat or drink. This could result in choking or aspiration.
STROKE
A stroke, sometimes called a brain attack, is a medical emergency caused by a blocked blood vessel or bleeding in the brain.
- Slurred or unintelligible speech
- Facial droop
- Numbness
- Weakness on one side of the body
- Difficulty walking or maintaining balance
- Loss of vision
- Severe headache
- Loss of consciousness
Stroke is a neurological emergency, so time is critical.
If you suspect a person is having a stroke, do the following:
- Immediately call 911.
- Help the person sit or lie down.
- Retrieve an AED and first aid kit.
- Record the time that neurologic symptoms were noted and the last time the person was free of symptoms.
- Be prepared to perform CPR if needed.
SEIZURES
Seizures result in abnormal body motion due to an irregular electrical discharge in the brain. Seizures can involve one or both sides of the body. Many seizures result in rhythmic jerking motions, but some seizures may result in a blank stare type of behavior. A person having a seizure may fall to the ground, bite their tongue, and lose control of bowel and bladder. Seizures are often accompanied by a brief period of unresponsiveness.
Causes of seizures or seizure-like activity include epilepsy, low blood sugar, head injury or trauma, heart disease, ingestion of a toxin, or heat-related illness.
When caring for a person experiencing a seizure, do the following:
- Help them to the ground if needed.
- Clear the area around them to prevent injury.
- Place a small pillow or towel under their head.
- Call 911.
After the seizure is over, do the following:
- Feel the person’s pulse. (Keep in mind that heart problems can cause seizure-like activity.)
- Position the person on their side to reduce the chance of choking on vomit. (Persons may throw up after a seizure.)
- Stay with them until help arrives.
Do not attempt to restrain a person having a seizure. Also, do not try to open their mouth or put anything between their teeth.
A victim experiencing an absence or staring-type seizure will have their eyes open but will not respond to you. These episodes are generally brief and not associated with jerky body motion or loss of consciousness. This type of event should be treated like any other seizure and a medical evaluation is warranted.
SHOCK
Shock can be caused by overwhelming infection, blood loss, severe allergic reaction, severe dehydration, or heart problems. When blood flow is significantly reduced, the body does not receive an adequate supply of oxygen, and shock occurs. Victims experiencing shock may lose consciousness or fail to respond.
Signs and symptoms of shock include:
- Poor skin color that is pale, gray, or bluish
- Dizziness and lightheadedness
- Nausea or vomiting
- Behavior change such as agitation, confusion, or unresponsiveness
- Clammy skin
When confronted with a person in shock, do the following:
- Activate the emergency response system by calling 911.
- Help the person lie down and elevate their legs.
- Cover the person with blankets to keep warm.
- Be prepared to perform CPR.
- Stay with the person until help arrives.


