Child CPR, AED, and Choking
Playlist includes 8 training videos
Children have breathing difficulties more often than they have actual heart problems. Therefore, it is important to begin CPR quickly and perform five sets of CPR for one rescuer or ten sets of CPR for two rescuers before going to get additional help. One set of CPR for one rescuer consists of 30 compressions and two breaths, and one set of CPR for two rescuers consists of 15 compressions and two breaths.
If available, make a second rescuer call 911/EMS and find an AED. Upon their return, work as a team and have them follow the AED prompts, apply the pads, and help you with CPR.
Provide CPR if the child is unresponsive and having trouble breathing.
Do the following when giving CPR to a child:
- Assess the safety of the scene and make sure the child is safe.
- Tap the child and ask loudly, “Are you okay?”
- Yell for help.
- Check the child’s breathing.
- If not responding and not breathing or only gasping, then give 2 minutes of CPR or five sets of 30 compressions (ten sets of 15 compressions for two rescuer).
- Get an AED and call 911/EMS.
- Resume CPR and give compressions and breaths.
Child CPR (1 year to puberty)
CPR is similar in adults and children. Giving breaths, pushing fast and hard on the chest, and early administration of CPR are the main goals. Children are those older than one year of age that who have not yet reached puberty. For the purposes of CPR, adult-sized children can be treated as adults.
Children who do not blink, speak, move, make a sound, or make any reaction to your efforts in awakening them are considered “unresponsive” or “not responding.”
Only use the “hands-only” CPR if you are an untrained rescuer. This means no breaths and only continuous compressions.
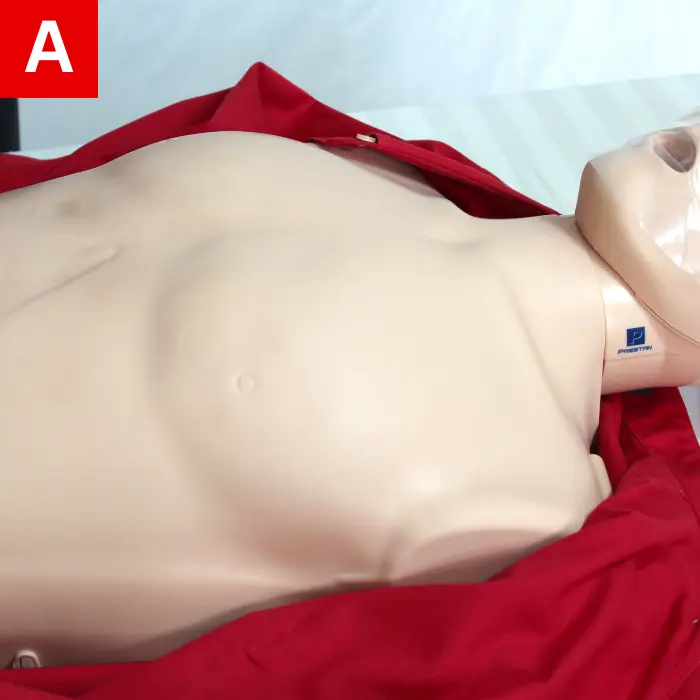
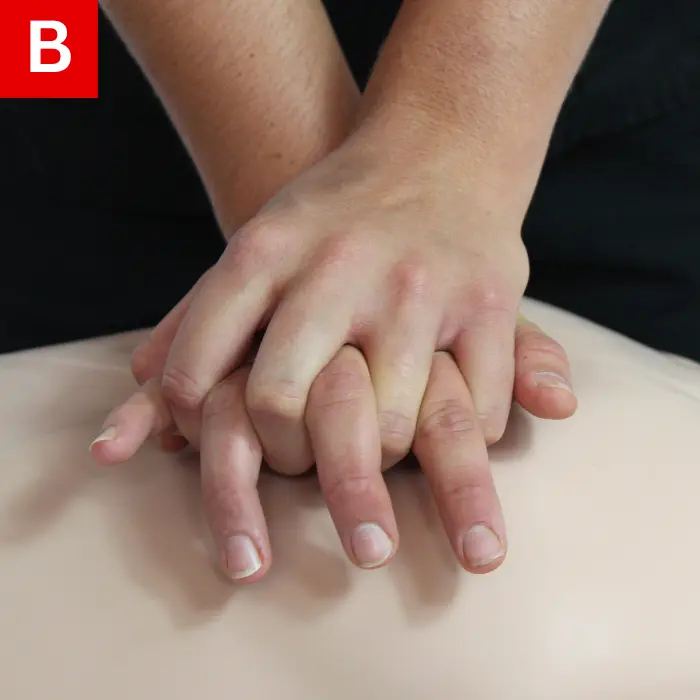
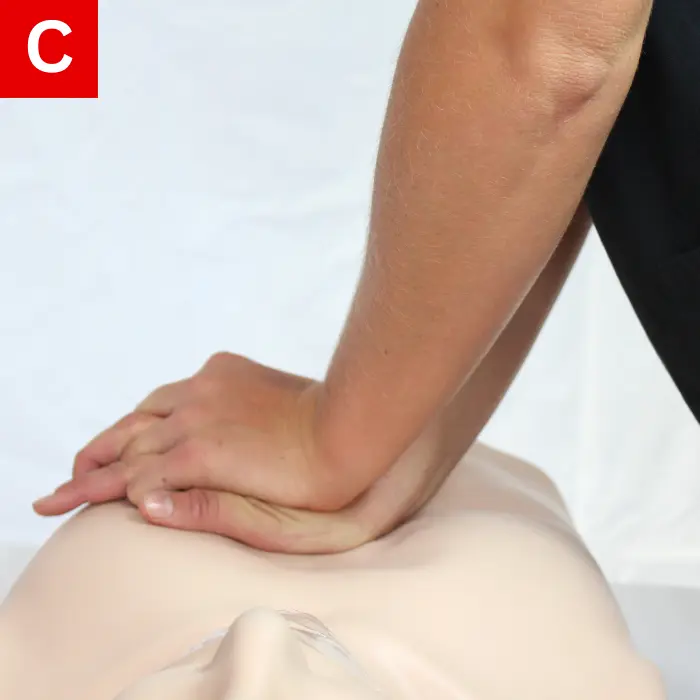
Figure 19
Compressions
It is common to be afraid of hurting the affected child when considering whether or not to do chest compressions. However, remember that the child will die without CPR.
Do the following to perform CPR on a child:
- Find a firm, flat surface to position the child on his or her back.
- Thick clothing at the neck and chest area must be opened or removed (Figure 19a).
- On the lower half of the breastbone, place the heel of one hand (Figure 19b).
- For at least one third the depth of the chest (about 2 inches or 5 cm in most children), push straight down. Deliver compressions at a rate of 100 to 120 beats per minute (Figure 19c).
- After each compression, allow the chest to fully recoil.
As CPR can become tiring, change roles with another person (if available) every two minutes. The pause between compressions must be minimized.
Giving Breaths
Breathing problems—not heart problems—are the most common cause of unresponsiveness in children. The most effective treatment is the prevention of choking or severe breathing problems due to untreated illness. The child can be helped with breaths during CPR. Cardiac arrest in children can be a result of severe breathing problems from a respiratory illness. The heart will beat irregularly or stop beating altogether due to a breathing problem in children who require CPR.
Absence of any breaths altogether, very shallow or sporadic breathing, and slow breathing are all signs of ineffective breathing. Children who are seemingly struggling to breathe must be given rescue breaths. The child’s chest will rise after a successful breath.
Do the following to open the child’s airway:
- Place a hand on their forehead (Figure 20a).
- On the bony part of their chin, place your fingers (Figure 20b).
- Lift their chin and tilt their head back gently (Figure 20c).
Do the following to give breaths:
- Pinch the child’s nose shut and hold their airway open (Figure 20d).
- Breathe deeply, then secure your mouth around the child’s mouth (Figure 20e).
- Watch their chest rise as you blow for one second into their mouth.
- Repeat with a second breath.
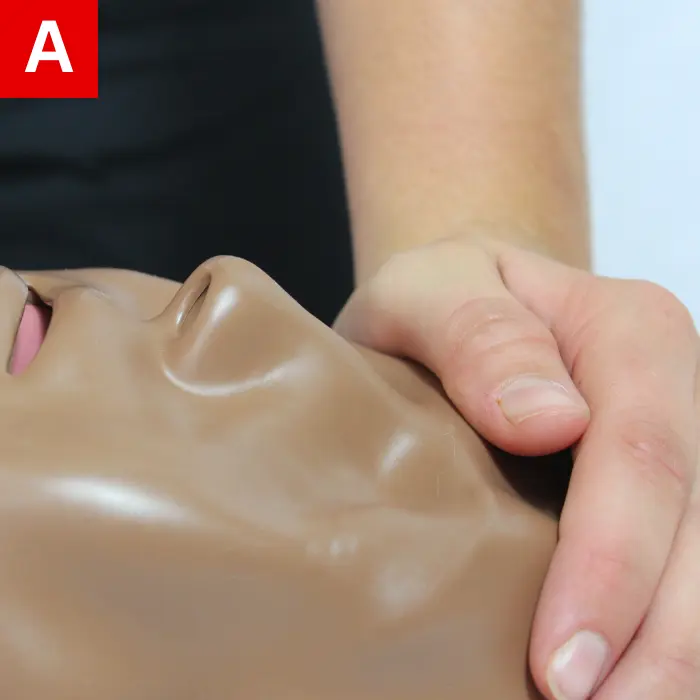
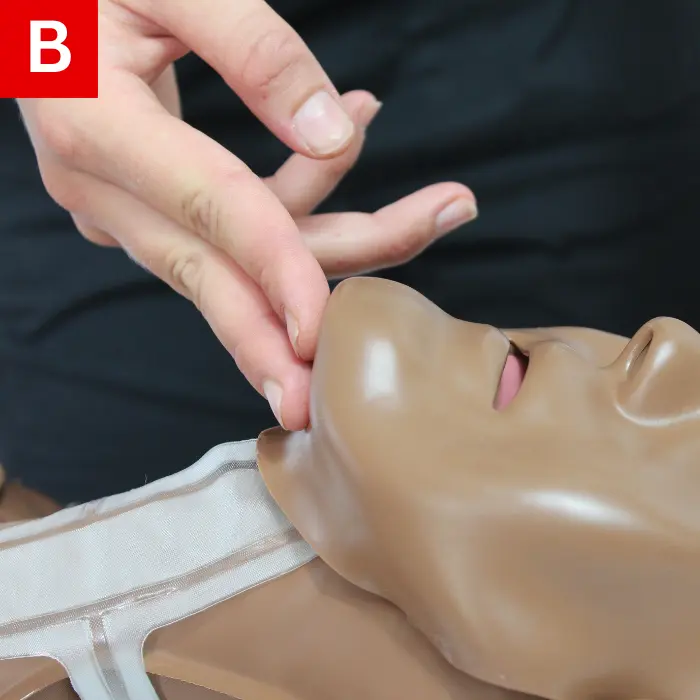



Figure 20
Reposition the airway if the chest does not rise. Let the child’s head go back to a normal position before repeating the head-tilt/chin-lift maneuver. Give another breath and look for the chest to rise.
Perform chest compressions without interruption. Do not allow any more than 10 seconds to give two breaths. Begin chest compressions again if the child’s chest fails to rise within 10 seconds.

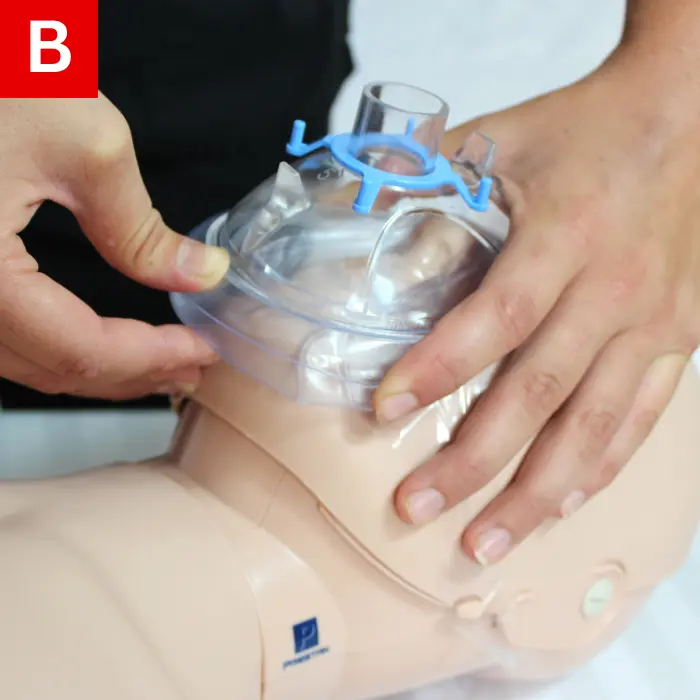

Figure 21
Mask Use
Generally, including the act of giving breaths, CPR is safe. However, use a mask whenever it is available. Fit the mask over the child’s nose and mouth. The pointed end of the mask should be fitted over the bridge of the child’s nose. The mask must fit properly; efforts to deliver breaths will be ineffective if the mask is too large because no proper seal is achieved.
Do the following when using a mask to give breaths to a child:
- Secure the mask over the child’s nose and mouth (Figure 21a).
- Perform the head-tilt/chin-lift maneuver to open the airway (Figure 21b).
- Ensure that there is a secure seal between the mask and the child’s face.
- Watch the chest rise as you give a breath for one second (Figure 21c).
- Deliver a second breath.

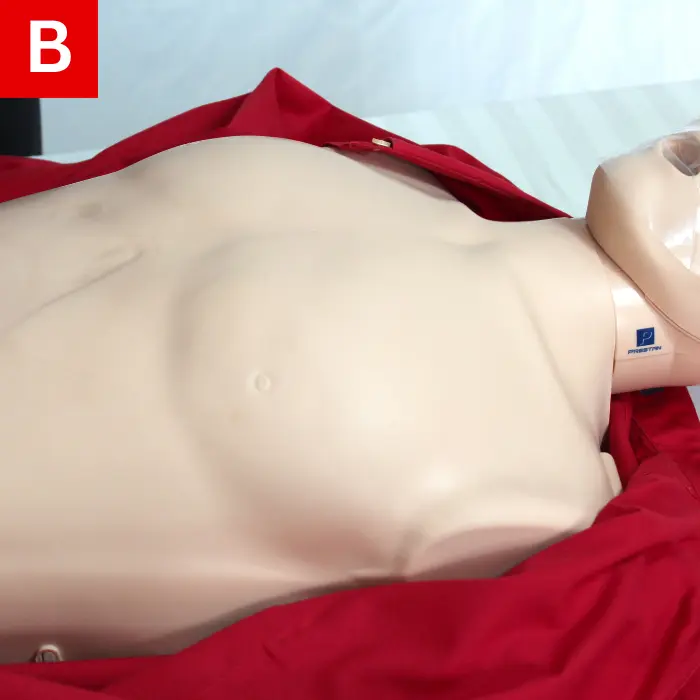
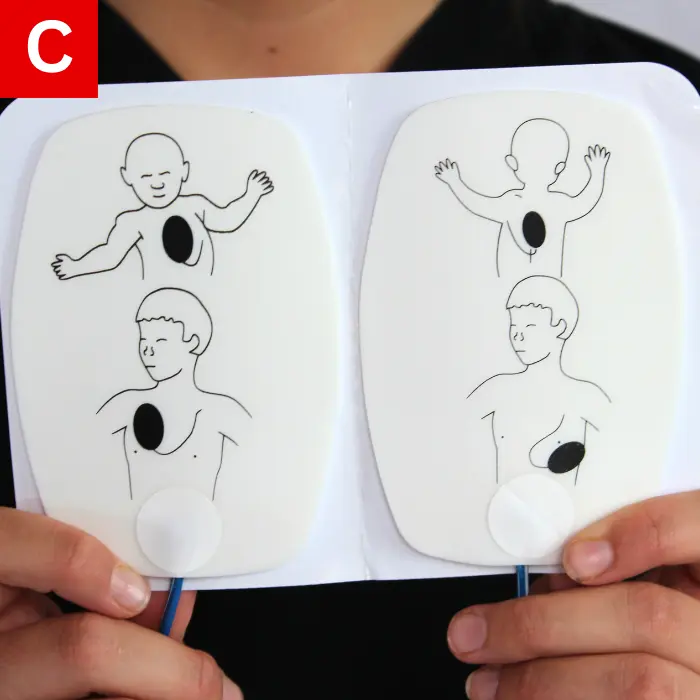



Figure 22
AED for Children
An AED can be used on children, and it should be administered as early as possible while not interfering with CPR. Using an AED on a child generally involves the same steps as using an AED on an adult. When the AED arrives on the scene, check it. Use pediatric pads if the child is younger than eight years of age (Figure 22c). However, if no pediatric pads are available, standard (adult) pads are acceptable. Do not let the pads touch or overlap when using standard pads. Because of this, if the child is small, one pad may have to be placed on the child’s back.
A pediatric shock can be delivered with some AEDs that have the appropriate switch or setting. For children younger than eight years of age, or less than 55 pounds (25 kg), turn this switch on (if available). An adult shock can be given if the available AED has no option for pediatric shocks. Start CPR immediately.
Do the following to use an AED on a child:
- Turn it on (Figure 22a).
- Reveal the child’s chest (Figure 22b).
- Apply the pads properly while ensuring that they do not touch (Figure 22c, Figure 22d).
- Connect the pads (Figure 22e).
- Clear the child; ensure that no one, including yourself, is touching the child.
- Check the rhythm.
- Follow the prompts: Shock Advised, No Shock Advised, Check Connection, etc.
- Begin compression again (Figure 22f).

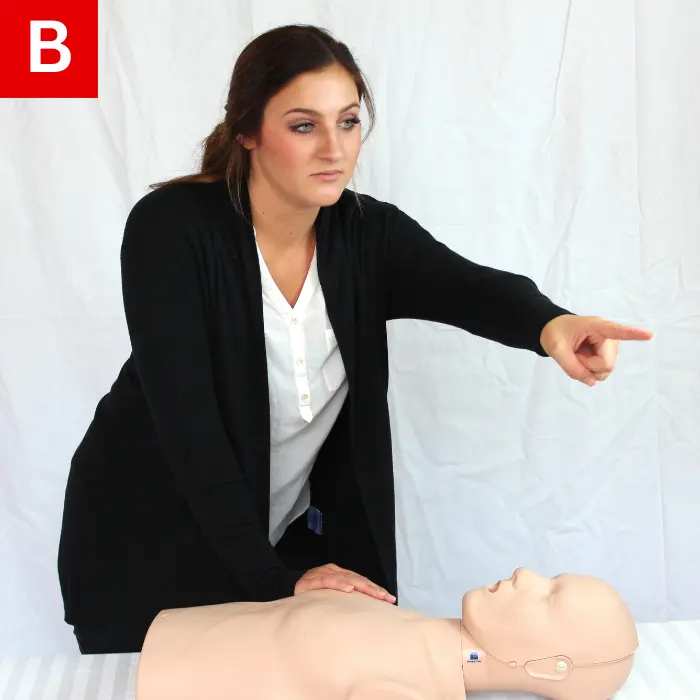

Figure 23
Activating EMS (Calling 911)
When approaching a child, be certain that the scene is safe. It will make the situation much worse if you become disabled or injured.
The child is considered unresponsive if he or she fails to respond to a tap and a loud question, like “Are you okay?”
(Figure 23a). Get an AED if possible and send another person to call 911/EMS after yelling for help (Figure 23b).
Check the child’s breathing after you have determined that he or she is unresponsive. Begin CPR immediately if the child is having trouble breathing or is only gasping, as gasping is generally ineffective, and often occurs in cardiac arrest (it is an abnormal sign).
Give five sets of 30 compressions and 2 breaths (about two minutes of CPR cycles) before leaving the child—and you should only leave the child if you are alone and cannot activate EMS using a cell phone at the scene. You can call 911/EMS without leaving the child in most cases, as most rescuers have cell phones on hand with speakerphones (Figure 23c).
Choking in Children
Choking can be either mild or severe. The airway is mildly blocked when the child can still cough and make sounds. Encourage them to cough and stand near them. If you are still worried about their breathing, call 911/EMS immediately.
The universal choking sign of clutching the throat, inability to speak, coughing without making a sound, and the inability to breathe are signs of severe blockage. Immediate action is required in cases such as these.
Determining whether choking is mild or severed is better understood in Table 2.
Yell for help and lay the child down if they stop responding. Begin CPR if there is no breathing. Open the airway and search for the foreign object after 15 compressions. Attempt to remove it and give a breath if the object is visible. Until more advanced help arrives or until the child recovers, continue applying CPR.
| Degree of Obstruction | Responsiveness | Rescuers Actions |
|---|---|---|
| Mild Obstruction |
|
|
| Severe Obstruction |
|
|
Table 2



Figure 24:
Heimlich Maneuver
Relief of Choking
For children who are choking, use abdominal thrusts as discussed in the adult section.
Do the following to relieve choking in a child:
- Ask if they are choking.
- Inform them that you are here to help.
- Wrap your arms around their body below the rib cage as you stand behind them (Figure 24a).
- Make a fist with your first hand and place it just above the navel (Figure 24b).
- With your other hand, grab your fist, then deliver quick upward thrusts (Figure 24c).
- Keep this up until the child stops responding, speaking or coughing is restored, or until the obstruction comes out and breathing is possible again.
Remove any foreign object that you may see in the child’s mouth. However, you risk pushing the object deeper into the airway if you blindly sweep the child’s mouth with your finger. Carefully observe their breathing by watching and feeling. Begin CPR and continue applying it until additional help comes if the child does not respond or begin breathing.
In cases of large children where your arms cannot wrap around their waist, perform chest thrusts, or perform abdominal thrusts with your fist on the breastbone.
A doctor should be consulted regarding any child who has experienced a severe choking event.
If the child stops responding, lay them down and yell for help. Check for breathing and begin CPR. After 30 compressions for one provider or 15 compressions for two, open the airway and look for a foreign object. If visible, remove it and attempt to give a breath. Continue CPR until the child recovers or more advanced help arrives.
