PEA vs Asystole: A Primer
PEA vs Asystole: A Primer

by Greta Kviklyte
Life Saver, AMC
Co-authored by Kim Murray, RN, M.S.
posted on Jan 27, 2020, at 2:41 pm
Pulseless electrical activity and asystole are deadly algorithms if left untreated. According to International Liaison Committee on Resuscitation (ILCOR), pulseless electrical activity refers to any rhythm that occurs without a detectable pulse; however, it excludes ventricular fibrillation (VF) and ventricular tachycardia (VT). Asystole is the more life-threatening arrhythmia. Also known as flatline, asystole occurs when all cardiac electrical activity stops and eventually presents itself in all dying individuals. With that in mind, these arrhythmias are not death sentences, provided appropriate action is taken in a timely manner.
We offer Online ACLS, PALS and BLS Certification and Renewal
For those new to the Advanced Cardiac Life Support (ACLS) algorithm, which is taught in courses across the country, such as the one available here, understanding the difference between these two rhythms is critical to maximizing patient treatment outcomes and avoiding adverse interventions during care.
What Exactly Is Asystole
Asystole does not occur without a cause. An event, trauma, injury, or literal electrical shock may stun the cardiac muscle and lead to asystole. This is known as secondary asystole. Asystole may also occur from a failure of the electrical nodes in the heart to generate an action potential (contraction), known as primary asystole. Primary asystole occurs when the sinoatrial (SA) node or atrioventricular (AV) node fails to trigger an action potential.

Remember that an action potential describes the depolarization of a cell in response to a stimulus. In this case, the SA node begins the depolarization process, triggering the depolarization of the right atrium. As the pulse moves downward, the right ventricle contracts pulsing blood back up through the pulmonary artery and to the lungs. When asystole occurs, the blockage of an action potential results in a loss of rhythm and heartbeat. With that in mind, primary systole may result from a unique type of bradycardia, bradyarrhythmia.
It may result from multiple forms of trauma, says EMedicine.Medicscape.com. For example, these conditions may contribute to asystole:
- Retrobulbar block
- Eye trauma
- Maxillofacial surgery
- Hypersensitive carotid sinus syndrome
- Glossopharyngeal neuralgia
Each of these conditions involves damage to the nerves surrounding the neck, face, and head.
Secondary asystole occurs when factors outside of the nerve system and the heart’s electrical conduction system fail. This results in a failure to generate any depolarization of cardiac tissue. In other words, the heart’s electrical system still functions, but it does not have the power to generate an action potential. The most common pathway to this form of asystole is hypoxia with metabolic acidosis.
Both types of asystole may also occur untreated ventricular fibrillation and before attempts to defibrillate.
What does that mean? Consider the reason asystole is an unshockable rhythm.
Why Is Asystole Unshockable
Health professionals dealing with someone in cardiac arrest tend to view medications and electrical stimulation (defibrillation) as the best ways to encourage return of spontaneous circulation (ROSC).
That is where the crux of ACLS lies. It provides a path for health professionals to encourage ROSC. It is that simple. If the heart’s electrical system cannot be moved into a rhythm capable of defibrillation or if it fails to achieve ROSC, the person dies.
What Exactly Is Pulseless Electrical Activity
Pulseless electrical activity, or more commonly referred to as PEA, can seem like a pre-emptive factor to asystole. Given that all cases resulting in cardiac arrest that do not achieve ROSC will eventually result in asystole, PEA can appear like nothing more than a warning sign. However, arrhythmia is much more complex.
PEA occurs when a major bodily problem leads to the inability of cardiac muscle to generate enough force to move blood through the chambers after depolarization. In other words, depolarization does occur, but for some reason, it is not strong enough to generate an actual heartbeat.
What Are the Causes of PEA
PEA is usually the result of a “profound cardiovascular problem,” says Medscape. For instance, hypovolemia, flow-restricting emboli, hypoxia, and metabolic conditions may lead to PEA. The full list of potential causes of PEA include all reversible causes of arrest, the H’s and T’s, which include and are listed online here:
- Hypoxia, which occurs following suffocation or failure of the lungs to properly oxygenate the blood.
- Hydrogen ion buildup, also known as acidosis, which may result from problems of the endocrine system or even non-medically supervised dietary changes.
- Hypo/hyperkalemia, which describes the buildup or decline in available potassium within the body, resulting in an imbalance of cellular tissues and problems generating or sustaining an action potential.
- Hypoglycemia, occurring from a rapid decline in blood serum glucose levels.
- Hypothermia, resulting from prolonged exposure to the elements, particularly the extreme cold.
- Tension pneumothorax, describing the changes within the pressure of the chest cavity, resulting in an equalization between exterior pressure and the inside of the chest wall, which makes it impossible to inhale.
- Tamponade of the heart, which may result from a tear of the coronary vessels, resulting from an obstruction or even an infection causing the protective covering of the heart, the pericardium, to fill with fluid.
- Toxins that lead to added strain on the body and may lead to the aforementioned causes of arrest, and toxins may also include severe allergen responses, such as anaphylactic shock.
- Thrombosis of the coronary vessels, preventing the perfusion of blood into cardiac tissues.
- Thrombosis of the pulmonary vessels, leading to a lack of adequate oxygenation of blood.
- Trauma, which may lead to any aforementioned cause of arrest.
Any H or T factor may lead to PEA. However, they have a few commonalities.
For instance, any condition may lead to decreased contractility of the heart. If the blood volume is insufficient, due to hemorrhage, any contraction will still not carry enough blood flow to support reoxygenation and provide nutrients through the coronary vessels. Meanwhile, depletion of ATP reserves, the energy-compound of cellular tissues, could lead to a failure of the heart to release after contract. Remember that ATP serves the as the release mechanism when it binds to sarcomeres after an action potential occurs within the muscle. Regardless, the most common reversible causes of PEA include hypovolemia, pump failure, and obstruction to circulation, such as choking or even trauma.
The Unique Case for PEA and Bradycardia in Pediatric Care
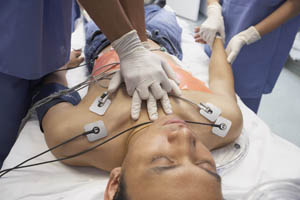
In fact, the ILCOR recommends the initiation of chest compressions and treating the rhythm as PEA once it declines below 60 BPM in children. This ensures adequate perfusion of tissues and promotes ROSC.
When Can a Shock Be Initiated
Both PEA and asystole remain non shockable rhythms. With that in mind, treating the causes of arrest should lead to a period where the rhythm enters a shockable state. Most importantly, continuation of the ACLS algorithm and working through its steps will include reassessment of possible causes of arrest and differential diagnoses. Thus, health professionals should maintain vigilance over when the rhythm converts from PEA or asystole to a shockable rhythm, such as ventricular or atrial fibrillation.
If a pulse is found, proven not be residual from chest compressions, review the electrocardiogram (EKG) reading.
For reference, both the EKG for ventricular fibrillation will have a squiggly appearance, and no discernable P-Wave, QRS complex, or T-Wave exists, but activity remains. The image below shows some differences among the waveforms:
When electrical activity moves beyond the level of fibrillation and appears to not represent any particular rhythm, it may be described as PEA. Most importantly, it is possible for any arrhythmia to become PEA when it does not generate a pulse and provide adequate perfusion. In these cases, it still carries the PEA diagnosis, but the cause of arrest is directly interfering with either the EKG’s accuracy or the cause of arrest, such as trauma, is beginning to inhibit the ability of the body to maintain a regular rhythm.
As soon as the body returns to a shockable rhythm, administer the shock, and proceed with the ACLS algorithm immediately. Time lost is brain lost, and the chances of positive outcomes dwindle. All health professionals need to learn to recognize and understand both PEA and asystole as unshockable and requiring immediate intervention. Furthermore, epinephrine in high-dose administration and traditional vasopressor use has been changed in recent years. Despite the changes, individual health facilities may follow additional protocols that supersede any recommendation by the ILCOR or other governing body. So, all providers should check with their respective employers or facilities to understand and know the appropriate ACLS protocol for those facilities.
What Is the Official Recommendation for Vasopressors During ACLS
When either PEA or asystole occurs, the ILCOR updated guidelines recommend against the use of atropine during ACLS. Atropine, which does have some evidentiary support for its use, was found to offer no therapeutic benefit to patients. Thus, the ILCOR removed it from the ACLS algorithm in its entirety. Meanwhile, standard dose epinephrine remains the vasopressor of choice for ACLS. With that in mind, an alternative vasopressor, such as vasopressin, may be used to supplement or replace epinephrine at the provider’s discretion.
This recommendation does require health professionals that do not meet the level of health provider, i.e. nurses, should defer judgement to the appropriate facility protocol or ordering physician, physician’s assistant, or nurse practitioner.
There does exist another instance in which high-dose epinephrine may be acceptable in the course of treatment of cardiac arrest. It involves administration to those suffering from anaphylactic shock. Since this shock is an immune system response to a given allergen, such as an insect sting or consumption of certain foods, high-dose epinephrine remains a strong measure to drive the cause of arrest for such instances—obstruction of the airway due to allergen response—into retreat. Thus, this is the one instance where high-dose epinephrine may be used in conjunction with the remainder of the ACLS algorithm to improve survival chances and positive outcomes.
Know the Difference Between PEA and Asystole
Lacking a pulse is different from asystole, despite the parallels between the connotation of both terms. Asystole is the flatline reading where all electrical activity within the heart ceases. PEA, on the other hand, may include randomized, fibrillation-like activity, but it does not rise to the level of actual fibrillation. Recognizing the difference between the two on an EKG and understanding how to treat a person in either rhythm is critical to maximizing chances of ROSC.
Have you ever been in a health facility where someone did not know how to determine between PEA and asystole, or have you ever considered a child’s care when his pulse drops below 60? If so, share your experiences and how you worked to help save lives today. Also, remember to enroll in a life-saving skills course, such as the one available here, to learn more about how to distinguish between asystole, PEA, and other life-threatening arrhythmias.



