Using PALS Megacodes to Increase Advocacy for Pediatric Health
Using PALS Megacodes to Increase Advocacy for Pediatric Health

by Greta Kviklyte
Life Saver, AMC
Co-authored by Kim Murray, RN, M.S.
posted on Dec 26, 2018, at 5:00 pm
The prevalence of cardiac arrest in children is less than the incidence of cardiac arrest in adults, and according to the American Heart Association (AHA), more than 5,000 children suffer cardiac arrest annually. Pediatric Advanced Life Support (PALS) may help reduce the prevalence of poor outcomes. To improve their skills, health care professionals should take part in training simulations, such as PALS Megacodes. They also need to know how to advocate for the care of children after cardiac arrest.
We offer Online PALS Certification and Renewal
The Epidemiology of Cardiac Arrest in Children
In-hospital cardiac arrest (IHCA) and out-of-hospital cardiac arrest (OHCA) may occur in children, but specific statistics are unavailable for the exact number of cases. Among children that suffer an OHCA, survival rate after treatment is extremely poor, 10 percent. However, survival rates after IHCA is significantly higher, ranging from 35 to 40.2 percent since 2012, reports AHAJournals.Org. Such survival rates mean more than one-half of children that suffer an IHCA do not survive to hospital discharge.
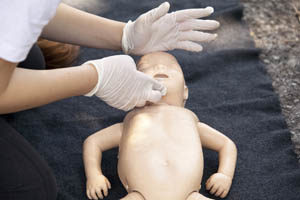
However, complications may arise, including subsequent IHCA. High-quality care as part of PALS in the immediate time after return of spontaneous circulation (ROSC) can help reduce poor outcomes.
PALS Megacodes Enhance Responsiveness to Children in Distress
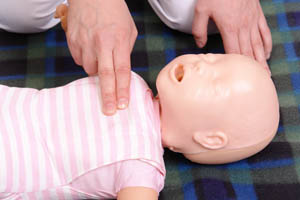
Time is of the essence in treating children after cardiac arrest, a time in which cardiac arrest is more likely to recur. This may be due to the confluence of factors contributing to arrest, including bradycardia. In PALS, any rhythm below 60 beats per minute warrants the initiation of the PALS algorithm and chest compressions.
The PALS Megacodes Bradycardia module focuses on this key aspect of caring for children. Although children may have a physical pulse below 60, decreased cardiac output increases the chances of tissue damage and death. Initiation of chest compressions ensures adequate perfusion of tissues, namely neural tissues.
While today’s electronic vital sign monitors can help health care professionals recognize bradycardia, it may still malfunction. Incorrect settings on the monitor may also lead to an assumption of stability. Unfortunately, these factors may result in a negative treatment outcome, including coma and permanent brain damage. The only way to curtail the risk is to understand when to start chest compressions through physical assessments. In addition, children may exhibit a rhythm above 60 on the monitor, but they may lack a physical pulse.
This is known as pulseless electrical activity (PEA), and it requires CPR. The bradycardia simulation emphasizes rhythms below 60 and the risk of PEA. Participants may need to interpret EKG readings in the simulation or identify the best course of action to achieve ROSC. Furthermore, the simulation runs comparable to the time spent assessing and acting upon cardiac arrest in children; they last between three and five minutes.
Simulations Offer an Opportunity to Understand Where Mistakes May Exist
 Following each answer, the participant receives an immediate notification of whether the selected choice is correct. Even in correct answers, a short dialogue box appears, explaining why it was the correct answer. For incorrect answers, the box reveals why it is incorrect and the rationale behind it. Although participants may read each answer’s description during the simulation, participants should at once move to the next question.
Following each answer, the participant receives an immediate notification of whether the selected choice is correct. Even in correct answers, a short dialogue box appears, explaining why it was the correct answer. For incorrect answers, the box reveals why it is incorrect and the rationale behind it. Although participants may read each answer’s description during the simulation, participants should at once move to the next question.
In a real-world situation, there is not time to second-guess responses and ask, “why?” Therefore, the end of the simulation reveals the participant’s score and a full breakdown of questions, including explanations. This is a great tool for helping participants know what parts of PALS to study.
Post-Arrest Treatment Standards Health Care Professionals Need to Know
When a child achieves ROSC, PALS does not end. Adult care, which is specific to cardiac arrest and its reversible causes, tends to close out the emergency response after ROSC. However, recent updates to the PALS algorithm advise health care professionals to continue to monitor the child for recurrence of symptoms and neurological deficits. While this is true in adults as well, the risk of PEA and poor perfusion from bradycardia in children warrant a heightened level of attention among health care professionals. As explained by ECCGuidelines.Heart.Org, health care professionals should follow take proactive action for post cardiac arrest care of the body’s major systems, including:
Respiratory System
Administering 100-percent oxygen to a child may be necessary in the course of PALS, but continued administration of 100-percent oxygen may result in worsening of condition. Oxyhemoglobin saturation of 100 percent is associated with poor clinical outcomes. Instead of administering 100-percent oxygen, health care professionals should titrate the dosage to lower the saturation level. The level should be less than 100 percent, but it should also be 94 percent or greater. This normalizes oxygen saturation without risking hypoxia.
Cardiovascular System
Monitoring the cardiovascular system is crucial following cardiac arrest, but it is important to remember PALS includes both cardiac arrest and trauma, even when not necessarily resulting in cardiac arrest. Respiratory arrest or traumatic brain injury may lead to the initiation of PALS. Moreover, vascular instability and dysfunction of cardiac tissue are common after ROSC in children. Therefore, it may be necessary to administer vasoactive drugs to increase function and perfusion. These medications include the following:
- Epinephrine – While low-dose administration of epinephrine, less than 0.3 mcg/kg per minute, may increase risk of tachycardia, decreased systemic vascular resistance, and potent inotropy, higher-dose administration may increase vasoconstriction. High-dose administration refers to dosages of more than 0.3 mcg/kg per minute. However, the response to administration of epinephrine may vary by patient and unique health conditions, so medications should be titrated to achieve the desired result. Also, epinephrine is preferable in infants with circulatory instability and decompensated shock.
- Norepinephrine – Norepinephrine is an effective treatment for promoting vasoconstriction when epinephrine is unavailable or does not work. Titrate the dosage based on need, such as sepsis, anaphylactic reactions, spinal injuries, or excessive vasodilation that is unresponsive to fluid administration.
- Dopamine – Dopamine is useful in treating shock that does not respond to fluids or when vascular resistance still is low. Dopamine dosage has a wide range of two to 20 mcg/kg per minute. Traditionally, dopamine use improves renal blood blow, but evidence to support this practice is subpar. As a result, it may not offer any advantage over other medications for renal blood flow. However, your facility may have a protocol for using dopamine for this purpose. Instead of advocating against its use, follow your facility’s protocol unless it would produce a higher risk to the patient. For instance, dopamine at infusion rates of greater than 20 mcg/kg has been associated with a higher oxygen consumption rate, so a child in respiratory distress may grow worse from administration of dopamine.
- Sodium Nitroprusside – Sodium nitroprusside decreases vascular resistance and reduces risk of hypotension. However, its complements the effects of other medications, such as an inotropes, which improve contractility in the cardiac tissue. Dosage of this medication will vary based on the manufacturer and availability in your facility, as well as recommendations from the treating physician.
- Inodilators – Inamrinone and milrinone increase cardiac output without increasing oxygen demand in cardiac tissue. Unfortunately, Inodilators have a long half-life and a marked delay in achieving optimum effects. For Inamrinone, the time is 18 hours, and it is 4.5 hours for milrinone. Furthermore, administration of fluids may be necessary to increase the effectiveness of these medications. Also, dosages for Inodilators will vary as well.
Neurologic System
The potential effect of cardiac arrest on neural tissue is severe. Prolonged deprivation of oxygen may lead to permanent injury and death. Infants may have a higher incidence of neurologic system damage due to the risk of sudden infant death syndrome (SIDS) and subsequent resuscitation. More importantly, infants with a known infection or suffering inflammation from illness have a higher risk of SIDS, reports the National Library of Medicine.
Unfortunately, researchers have not found a definitive pathogen responsible for SIDS. This correlation simply means that health care professionals should take extra care in providing PALS following resuscitation of infants, especially those in suspected cases of SIDS. It can seem confusing, but it is possible to revive an infant that has stopped breathing without explanation, which would have otherwise resulted in a SIDS’ cause of death. Now, resuscitation from SIDS has a significantly higher risk of poor oxygen perfusion and higher PaCO2 levels. As a result of acidosis from higher levels, fever may occur.
Fever is one of the factors associated with inflammation and damage to neural tissue. It also contributes to the release of unbound oxygen atoms in the bloodstream, which may cause tissue damage. In fact, unbound oxygen atoms have another name, free radicals, and they may increase risk of neural damage too. However, targeted temperature management (TTM), involving the use of induced hypothermia, may serve a protective effect against permanent neural damage.
The 2015 PALS guidelines did not place a specific recommendation on the use for or against TTM for infants and children remaining comatose after OHCA. Since SIDS is a type of OHCA, the use of TTM is at the discretion of the treating physician. Infants and children may be maintained in a state of normothermia, the typical body temperature, for a period of five days. Alternatively, they may receive 48 hours of hypothermia, followed by three days of normothermia.
The 2015 update did recommend against the use of TTM for infants and children in a comatose state after IHCA. This is due to the increased likelihood that an immediate response occurred when the child stopped breathing or entered cardiac arrest. Meanwhile, an OHCA includes a risk for a period when the parents or caregivers were unaware that a problem had arisen.
Health care professionals must recognize that outcomes from OHCA may improve with the use of TTM. Of course, facility-specific guidelines and limitations may apply, but health care professionals can advocate for the use of TTM in OHCA in children.
Renal System
Following cardiac arrest, health care professionals must monitor the urine output to identify and manage prerenal conditions. Urine output should be greater than one mL/kg for infants and children or greater than 30 mL/hour in adolescents. Decreased urine output warrants immediate adjustment of medication dosages to improve renal function. Until a full evaluation of kidney function has been conducted, avoid administering unnecessary, nephrotoxic medications.
Participate in PALS Training Simulations Now to Improve Your Skills
Situations may arise where health care professionals do not know how to respond. Unique circumstances and risks may lead to unorthodox treatment measures. However, health care professionals that completely understand the PALS algorithm and have taken part in training scenarios are better-equipped to improve the chances of positive treatment outcomes.
Ensuring positive treatment outcomes means keeping a close eye over children that have suffered cardiac arrest after ROSC and knowing when innovative treatment options may help. Health care professionals should know what type of medications to use to improve cardiac output and recognize the life-saving potential of TTM. Unfortunately, the costs of TTM equipment to administer and monitor children after OHCA may make this treatment inaccessible, especially among smaller hospitals and care settings. Therefore, health care professionals should make every effort to ensure they can respond at once with the right life-saving measures, and this includes immediately beginning chest compressions when needed and practicing their PALS skills in PALS Megacodes.
Put your skills to the test in the online simulation now, and share your results, along with this article, to social media. Megacodes empower health care professionals to save lives, so be part of the solution to improve positive patient outcomes today.



